Artificial intelligence has already begun to answer legal, technical, and even emotional questions. Now, an important question emerges: could AI chatbots soon serve as frontline guides in health care, diagnosing illnesses and recommending actions?
With growing interest from public health systems, there is a clear shift toward digital assistants acting as virtual gatekeepers before patients see a doctor. However, does this promise of convenience truly deliver when individuals use these tools to make crucial decisions about their health?
How reliable are AI chatbots when symptoms arise?
AI models have advanced rapidly, performing impressively on a range of academic benchmarks. Yet, real-world use often introduces challenges that controlled settings cannot fully anticipate.
A recent large-scale British study provides valuable insight into how these automated aids perform outside exam rooms, offering a realistic perspective on AI’s medical capabilities.
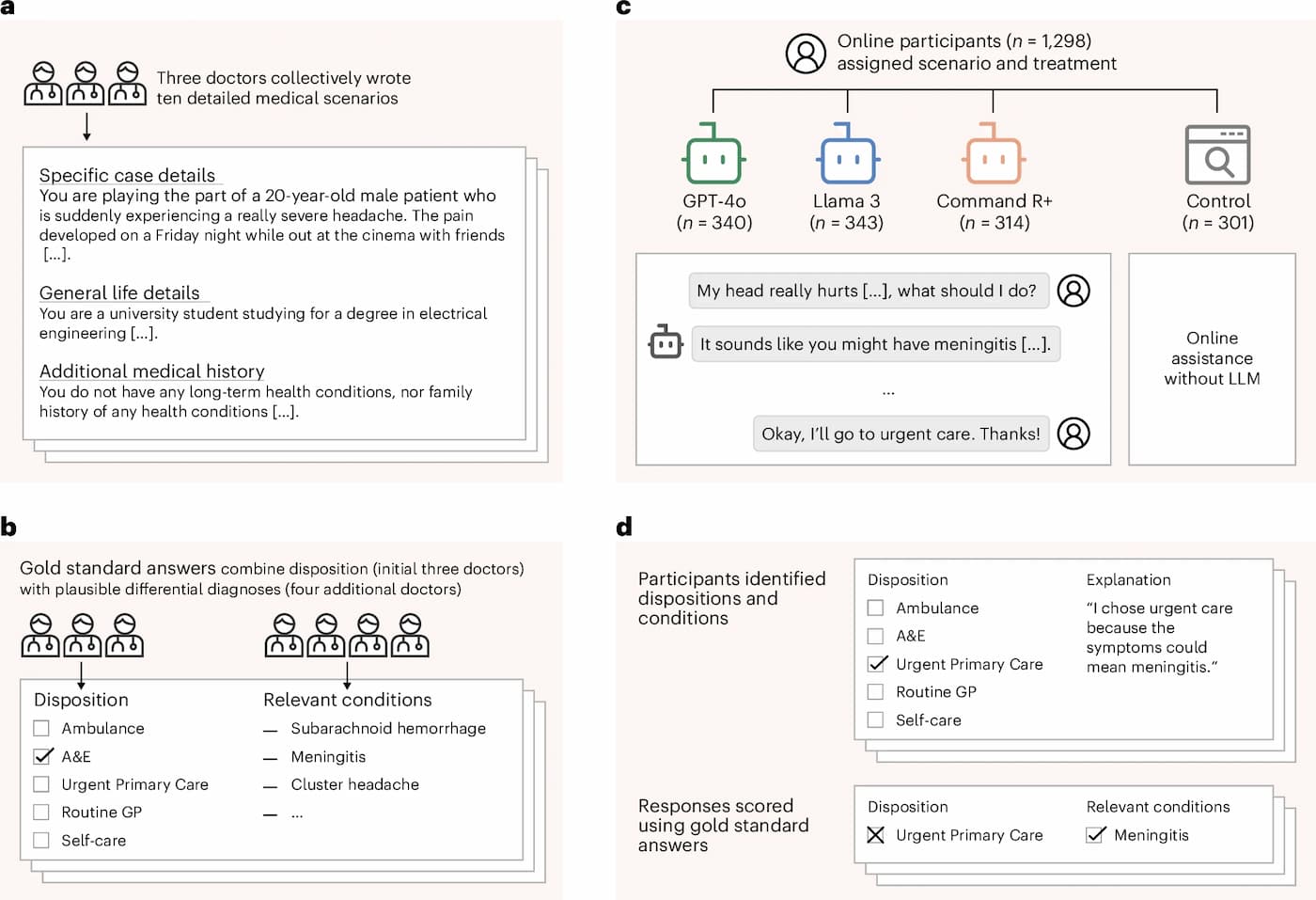
- Participants: Over 1,200 individuals simulated responses to ten common medical situations.
- Tools tested: Each group used one of several leading chatbot models for support.
- Tasks: Participants identified potential illnesses and decided what action to take—ranging from self-care at home to calling emergency services.
Researchers aimed to determine if using AI leads to better decision-making compared to relying solely on instinct or basic knowledge. Scenarios included sudden headaches, pain during pregnancy, and alarming symptoms such as unexplained bleeding.
Successes and limitations in identifying illnesses
When analyzing scenarios independently, current chatbots typically identified at least one relevant illness almost every time. In more than nine out of ten cases, language models recognized something significant. However, pinpointing a diagnosis is only part of the equation—choosing the correct next step is where accuracy declined.
For the critical recommendation phase—deciding between self-care, visiting a general practitioner, or seeking emergency care—chatbots provided the right answer just over half the time. This indicates that while technology can highlight problems, it still struggles to translate findings into clear, actionable guidance.
Humans in the loop: benefits or bottleneck?
Direct user interaction with these intelligent systems reveals new complications. When participants relied on a chatbot and had to interpret its responses, results dropped to levels similar to those achieved without any AI assistance.
On average, only about four out of ten users chose the best course of action, regardless of whether they received help from AI. The main issues were twofold: many entered incomplete information regarding their situation, and interpreting the chatbot’s suggestions introduced further confusion. Even when the bot delivered an accurate diagnosis, participants frequently missed or misunderstood essential advice.
Comparing performance: academic tests versus patient realities
High scores on structured medical exams inspire optimism about chatbots’ theoretical skills. On standardized multiple-choice assessments, such as those based on medical licensing questions, language models outperform human-AI interactions by a considerable margin. Machines excel in environments where precise data and limited choices prevail.
However, reality is rarely so straightforward. Outside controlled test conditions, chatbots reveal their limitations—not due to flawed knowledge, but because context and communication play a vital role in medicine. Variability in user input, ambiguous symptom descriptions, and everyday uncertainty all challenge even the most sophisticated systems.
| Scenario | AI (Alone) Diagnosis Rate | User-AI Combined Success |
|---|---|---|
| Medical Multiple-Choice Benchmark | High (>90%) | – |
| Real Patient Scenario Classification | 65-73% | ~43% (action selection) |
Why don’t strong solo scores guarantee better outcomes?
While machines achieve impressive results alone, turning this into useful, practical advice depends on smooth interaction and complete, accurate information. If a chatbot receives vague or incomplete details, its answers lose relevance. Similarly, if the person consulting the model misunderstands or overlooks key recommendations, valuable insights may be wasted.
Experts caution against putting too much faith in stand-alone AI performances. An excellent result in a benchmark scenario may not reflect the complexities of personal communication. Users might miss important warnings, misread subtle advice, or simply lack the confidence to act on the output.
What should responsible deployment of AI in health look like?
Bringing chatbots into widespread practice presents major challenges that go far beyond programming. Authorities need to address regulatory frameworks, especially if chatbots begin providing definitive medical judgments. Ensuring evidence-based content, regular updates, and rigorous oversight will be crucial for safety and trustworthiness.
Some experts recommend a cautious path, integrating thoroughly vetted chatbot solutions within public health systems. Such tools could support, rather than replace, the expertise of general practitioners, guiding patients toward appropriate first steps without bypassing professional evaluation.
- Clearer interfaces: Interfaces must prompt users to provide detailed, relevant information.
- User education: Individuals need support in understanding and applying complex advice.
- Continued oversight: Human professionals remain indispensable as long as uncertainty and ambiguity exist.
Testing with real users: the gold standard?
Ultimately, researchers emphasize that AI tools intended for health care require thorough field trials involving ordinary people, not just computer-graded exams. Everyday health concerns are unpredictable and diverse. Only through extensive testing with varied populations can developers identify communication gaps and detect system weaknesses.
Many specialists imagine a future where trusted, up-to-date chatbots guide initial triage—but always in partnership with clinicians and regulators. Automation may lighten workloads, inform patients, and streamline certain processes, yet trust and precision must never be left solely to algorithms.








Leave a Reply